Hodgkin Lymphoma: Types, Risk Factors, Symptoms, Signs, Diagnosis and Prognosis
What is Hodgkin Lymphoma? Understanding the Hodgkin Lymphoma (Hodgkin's Disease)
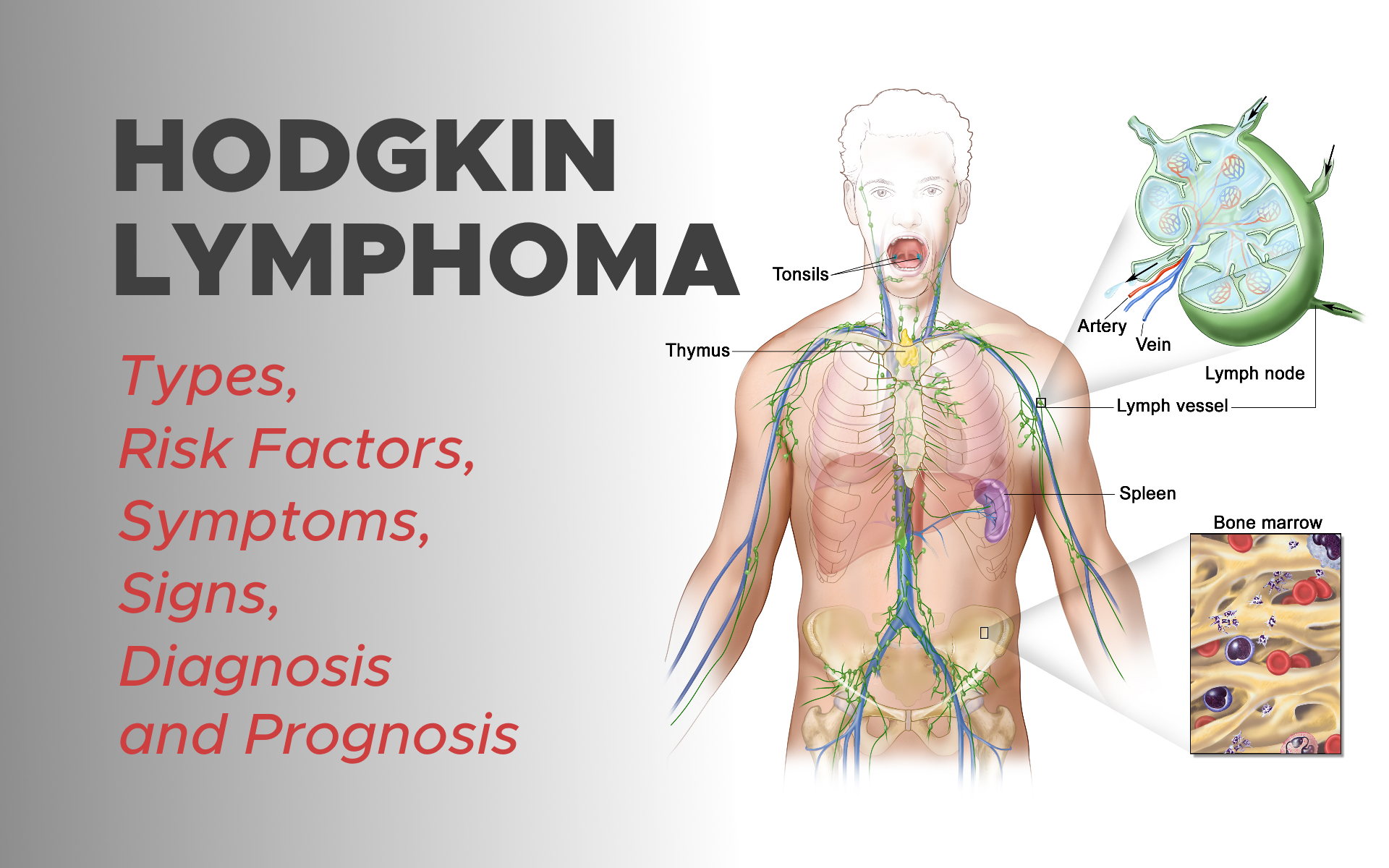
Lymphatic System
The lymphatic system is made up of lymph nodes, lymphatic organs, and lymphatic vessels. Its job is to fight infection and disease. The lymphatic system carries lymph, a colorless fluid that contains lymphocytes. Lymphocytes are a type of white blood cell that makes up part of the immune system. Lymphatic vessels are thin tubes that branch out to all parts of the body.
There are several types of lymphocytes, including:
- B cells, or B-lymphocytes, make antibodies to fight bacteria and other infections.
- T cells, or T-lymphocytes, kill bacteria, viruses, fungi, and abnormal cells and trigger the B cells to make antibodies.
In a routine complete blood count (CBC) test, lymphocytes are measured in the blood as part of the white blood cell count.
Groups of bean-shaped organs called lymph nodes are located throughout the body in different areas within the lymphatic system. The largest groups of lymph nodes are found in the chest, abdomen, groin, pelvis, underarms, and neck.
Other parts of the lymphatic system include the:
- Spleen, which is located in the left upper abdomen, under the rib cage. The spleen makes lymphocytes and filters the blood.
- Thymus, which is an organ located behind the breastbone. The thymus plays an important role in the development of T cells.
- Tonsils, which are located in the throat. The tonsils help trap bacteria entering through the mouth or nose.
Hodgkin Lymphoma (Hodgkin’s Disease)
Lymphoma is a cancer of the lymphatic system. Hodgkin lymphoma, which used to be called Hodgkin’s disease, is 1 of many types of lymphoma. Lymphoma begins when healthy cells in the lymphatic system change and grow out of control. This uncontrolled growth may form a tumor, involve many parts of the lymphatic system, or spread to other parts of the body.
Hodgkin lymphoma (Hodgkin’s Disease) most commonly affects lymph nodes in the neck or the area between the lungs and behind the breastbone. It can also begin in groups of lymph nodes under an arm, in the groin, or the abdomen or pelvis.
If Hodgkin lymphoma spreads, the most common locations where it spreads are the lung, spleen, liver, bone marrow, or bone. Hodgkin lymphoma can spread to other parts of the body, but this is unusual.
Types of Hodgkin Lymphoma (Hodgkin’s Disease)
There are different types of Hodgkin lymphoma. It is important to know the type because this may affect how the cancer is treated. Doctors determine the type of Hodgkin lymphoma based on how the cells look under a microscope and whether the cells contain certain abnormal proteins. These cells are taken using a tissue biopsy.
The American Joint Committee on Cancer (AJCC) recognizes 2 major categories of Hodgkin lymphoma: classic Hodgkin lymphoma and nodular lymphocyte-predominant Hodgkin lymphoma.
1. Classic Hodgkin lymphoma (cHL)
Classic Hodgkin lymphoma (cHL) is the most common type of Hodgkin lymphoma. About 95% of cases of Hodgkin lymphoma are within the classic Hodgkin lymphoma (cHL) category. Classic Hodgkin lymphoma (cHL) is diagnosed when certain abnormal lymphocytes, known as Reed-Sternberg cells, are found. cHL is divided into 4 subtypes, based on the appearance of the lymph node structure and cells:
a. Nodular Sclerosis Hodgkin Lymphoma
Nodular sclerosis Hodgkin lymphoma is the most common subtype of classic Hodgkin lymphoma (cHL). It affects up to 80% of people diagnosed with classic Hodgkin lymphoma (cHL). Nodular sclerosis Hodgkin lymphoma is most common in young adults, especially women.
In addition to Reed-Sternberg cells, there are bands of connective tissue (called fibrosis) found in the lymph node. The presence of these bands can help diagnose this type of Hodgkin lymphoma. This type of lymphoma often affects the lymph nodes in the central part of the chest, called the mediastinum.
b. Lymphocyte-Rich Classic Hodgkin Lymphoma
About 6% of people with classic Hodgkin lymphoma (cHL) are diagnosed with lymphocyte-rich classic Hodgkin lymphoma. It is more common in men and usually affects areas other than the mediastinum. In addition to Reed-Sternberg cells, the lymph node tissue contains many normal lymphocytes.
c. Mixed Cellularity Hodgkin Lymphoma
This subtype of classic Hodgkin lymphoma (cHL) occurs most often in older adults. It sometimes develops in the abdomen and carries many different cell types, including large numbers of Reed-Sternberg cells.
d. Lymphocyte-Depleted Hodgkin Lymphoma
Lymphocyte-depleted Hodgkin lymphoma is the least common subtype of classic Hodgkin lymphoma (cHL). Only about 1% of people with classic Hodgkin lymphoma (cHL) have this subtype. It is most common in older adults; people with the human immunodeficiency virus (HIV), the virus that causes autoimmune deficiency syndrome (AIDS); and people in non-industrialized countries. The lymph node contains almost all Reed-Sternberg cells.
2. Nodular Lymphocyte Predominant Hodgkin Lymphoma
About 5% of people with Hodgkin lymphoma have nodular lymphocyte-predominant Hodgkin lymphoma. It often develops in the lymph nodes in the neck, groin, or armpit. It is most common in younger people.
Nodular lymphocyte-predominant Hodgkin lymphoma is more similar to B-cell non-Hodgkin lymphoma. People with this type of Hodgkin lymphoma have large cells in the affected area called “popcorn cells” or “LP cells” that have a marker called CD20 on their surface. CD20 is a protein that is usually found in people diagnosed with B-cell non-Hodgkin lymphoma.
Nodular lymphocyte-predominant Hodgkin lymphoma is often treated differently from classic Hodgkin lymphoma (cHL). Some people with nodular lymphocyte-predominant Hodgkin lymphoma do not need treatment right away, while others may benefit from a treatment plan that includes radiation therapy, chemotherapy, or a monoclonal antibody called rituximab (Rituxan).
People with nodular lymphocyte-predominant Hodgkin lymphoma tend to have a very good prognosis. This means the treatment if needed, has a very good chance of being successful and helps the patient recover.
However, a small number of people with nodular lymphocyte-predominant Hodgkin lymphoma may develop a more aggressive type of non-Hodgkin lymphoma called diffuse large B-cell lymphoma through a process called transformation.
Risk Factors of Hodgkin Lymphoma
A risk factor is anything that increases a person’s chance of developing cancer. Although risk factors often influence the development of cancer, most do not directly cause cancer.
Some people with several risk factors never develop cancer, while others with no known risk factors do develop cancer. Knowing your risk factors and talking about them with your doctor may help you make more informed lifestyle and health care choices.
The exact cause of Hodgkin lymphoma is not known, but the following factors may raise a person’s risk of developing Hodgkin lymphoma:
- People between the ages of 15 and 40 and people older than 55 are more likely to develop Hodgkin lymphoma.
- In general, men are slightly more likely to develop Hodgkin lymphoma than women, although the nodular sclerosis subtype is more common in women.
- Family history. Brothers and sisters of people with Hodgkin lymphoma have a higher chance of developing the disease, although the increase in risk is small.
- Virus exposure. The Epstein-Barr virus (EBV) causes infectious mononucleosis, often called “mono.” Nearly all adult Americans and many others around the world have an EBV infection. About 20% to 25% of people with classic Hodgkin lymphoma (cHL) in the United States have lymphoma cells that test positive for EBV. Although a person’s immune system response to infection with EBV may be important in the development of Hodgkin lymphoma, doctors still do not understand why, when so many people have been infected with EBV, relatively very few people ever develop Hodgkin lymphoma. People with HIV also have a higher risk of developing Hodgkin lymphoma, particularly lymphocyte-depleted Hodgkin lymphoma.
Symptoms and Signs of Hodgkin Lymphoma
People with Hodgkin lymphoma may experience the following symptoms or signs. Sometimes, people with Hodgkin lymphoma do not have any of these changes. Or, the cause of a symptom may be a different medical condition that is not cancer.
Common symptoms or signs caused by Hodgkin lymphoma include:
- Painless swelling of lymph nodes in the neck, underarm, or groin area that does not go away within a few weeks
- Unexplained fever that does not go away
- Unexplained weight loss
- Night sweats, usually drenching
- Pruritus, a generalized itching that may be severe
- Fatigue
- Pain in the lymph nodes triggered by drinking alcohol
- Shortness of breath, cough, or chest discomfort may be caused if lymph nodes in the chest are affected
If you are concerned about any changes you experience, please talk with your doctor. Your doctor will ask how long and how often you’ve been experiencing the symptom(s), in addition to other questions. This is to help figure out the cause of the problem, called a diagnosis.
If the diagnosis is Hodgkin lymphoma, the doctor may also use certain symptoms to help describe the disease in a process known as staging. Each stage may be subdivided into “A” and “B” categories.
A means that a person has not experienced B symptoms, which are listed below.
B means that a person has experienced 1 or more of the following symptoms:
- Unexplained weight loss of more than 10% of original body weight during the 6 months before diagnosis.
- Unexplained fever, with temperatures above 100.4°F (38°C).
- Drenching night sweats. Many people with Hodgkin lymphoma say their nightclothes or the sheets on the bed were so wet they needed to be changed during the night. Sometimes, heavy sweating occurs during the day.
If cancer is diagnosed, relieving symptoms remains an important part of cancer care and treatment. This may be called palliative care or supportive care.
It is often started soon after diagnosis and continued throughout treatment. Be sure to talk with your health care team about the symptoms you experience, including any new symptoms or a change in symptoms.
Diagnosis of Hodgkin Lymphoma
Doctors use many tests to find or diagnose, cancer. They also do tests to learn if cancer has spread to another part of the body from where it started. If this happens, it is called metastasis. For example, imaging tests can show if cancer has spread. Imaging tests show pictures of the inside of the body. Doctors may also do tests to learn which treatments could work best.
For most types of cancer, a biopsy is the only sure way for the doctor to know if an area of the body has cancer. In a biopsy, the doctor takes a small sample of tissue for testing in a laboratory. If a biopsy is not possible, the doctor may suggest other tests that will help make a diagnosis.
This section describes options for diagnosing Hodgkin lymphoma. Your doctor may consider these factors when choosing a diagnostic test:
- The type of cancer suspected
- Your signs and symptoms
- Your age and general health
- The results of earlier medical tests
The following tests may be used to help diagnose Hodgkin lymphoma. Not all tests listed below will be used for every person.
1. Medical History and Physical Examination
The doctor will ask detailed questions about your medical history and do a physical examination, which can identify whether the person has experienced some typical symptoms of Hodgkin lymphoma, such as night sweats, fevers, and enlarged lymph nodes or spleen.
2. Biopsy
A biopsy is the removal of a small amount of tissue for examination under a microscope. Other tests can suggest that cancer is present, but Hodgkin lymphoma can only be diagnosed after a biopsy of affected tissue, preferably by removal (or excision) of a lymph node.
Most commonly, this will be an affected lymph node in the neck, under the arm, or in the groin. If there are no lymph nodes in these areas, a biopsy of other lymph nodes, such as those in the center of the chest, may be necessary.
This type of biopsy usually requires minor surgery using a procedure called mediastinoscopy. A thin, lighted tube with a camera and a cutting tool on the end is inserted into the chest through a small cut made just above the breastbone.
It may also be possible to do a biopsy using a core needle. Doctors most commonly use ultrasound or a computed tomography (CT or CAT) scan (see below) to help guide the needle to the correct location.
A pathologist then analyzes the tissue sample(s) removed during the biopsy. A pathologist is a doctor who specializes in interpreting laboratory tests and evaluating cells, tissues, and organs to diagnose disease. A hematopathologist is a doctor who has received additional training in blood diseases and blood cancer diagnosis.
The biopsy sample must be large enough to allow the pathologist to make an accurate diagnosis and determine the subtype of Hodgkin lymphoma. If the first biopsy does not have enough tissue to diagnose lymphoma, a second larger biopsy may be needed.
As described in the introduction, a biopsy of classic Hodgkin lymphoma (cHL) usually has Reed-Sternberg cells. For people with nodular lymphocyte-predominant Hodgkin lymphoma, the Reed-Sternberg cells often look different and are called “LP” cells. In contrast to classic Reed-Sternberg cells, LP cancer cells have a protein on their surface called CD20.
Once Hodgkin lymphoma is diagnosed, other tests can help find out the extent of the disease, the stage, and other information to help the doctors plan treatment. These tests include:
3. Laboratory Tests
Blood tests may include a complete blood count (CBC) and an analysis of the different types of white blood cells, in addition to the erythrocyte sedimentation rate (ESR or “sed rate”) and liver and kidney function tests. Blood tests alone cannot detect Hodgkin lymphoma.
4. Computed Tomography (CT or CAT) Scan
A CT scan takes pictures of the inside of the body using x-rays taken from different angles. A computer combines these pictures into a detailed, 3-dimensional image that shows any abnormalities, such as enlarged lymph nodes, or tumors.
A CT scan of the chest, abdomen, and pelvis can help find cancer that has spread to other parts of the body. A special dye called a contrast medium is usually given before the scan to improve the details of the images.
This dye can be injected into a patient’s vein, along with an oral liquid to swallow to help take images of the stomach and intestines. People with a history of kidney disease or poor kidney function should not receive a contrast medium given into a vein (intravenously or IV).
5. Positron Emission Tomography (PET) or PET-CT Scan
A PET scan is usually combined with a CT scan, called a PET-CT scan. However, you may hear your doctor refer to this procedure just as a PET scan. A PET scan is a way to create pictures of organs and tissues inside the body.
A small amount of a radioactive sugar substance is injected into the patient’s vein. This sugar substance is taken up by cells that use the most energy. Because cancer tends to use energy actively, it absorbs more of the radioactive substance.
A scanner then detects this substance to produce images of the inside of the body. PET-CT scans may be used to determine the stage of Hodgkin lymphoma. PET-CT scans may also be used to see how the lymphoma is responding to treatment.
6. Magnetic Resonance Imaging (MRI)
An MRI uses magnetic fields, not x-rays, to produce detailed images of the body. A special dye called a contrast medium is given before the scan to create a clearer picture. This dye can be injected into a patient’s vein. This test is sometimes used for Hodgkin lymphoma.
7. Lung Function Tests
Also called pulmonary function tests or PFTs, lung function tests evaluate how much air the lungs can hold, how quickly air can move in and out of the lungs, and how well the lungs add oxygen and remove carbon dioxide from the blood. These tests may be done if a person’s treatment plan includes chemotherapy with certain drugs that could affect the lungs.
8. Heart Evaluation
A heart evaluation, including an echocardiogram (ECHO)or a multigated acquisition (MUGA) scan, may be used to check the function of the heart if specific types of chemotherapy will be included in a person’s treatment plan.
9. Bone Marrow Aspiration and Biopsy
These 2 procedures are similar and often done at the same time to examine the bone marrow. Bone marrow is the soft, spongy tissue found inside the center of bones. It has both a solid and a liquid part. A bone marrow aspiration removes a sample of the fluid with a needle.
A bone marrow biopsy is the removal of a small amount of solid tissue using a needle. A pathologist then analyzes the sample(s). These bone marrow procedures have been mostly replaced with PET-CT scans, but they may still be done in certain situations.
Statistics and Prognosis of Hodgkin Lymphoma
This year, an estimated 8,830 people (4,830 men and 4,000 women) in the United States will be diagnosed with Hodgkin lymphoma. From 2008 to 2017, the number of people diagnosed with this disease dropped by around 2% each year.
The survival rate has been going up since around 1975, thanks to treatment improvements. From 2009 to 2018, the death rate dropped 4% annually.
Hodgkin lymphoma affects both children and adults. It is most common in 2 age groups.
- The first group is people in early adulthood, particularly people in their 20s.
- The second is people older than 55. The average age of diagnosis is 39.
Although the disease is rare in children younger than 5, it is the most commonly diagnosed cancer in teens ages 15 to 19. The disease accounts for 12% of all cancer cases in this age group.
The 5-year survival rate tells you what percent of people live at least 5 years after the cancer is found. Percent means how many out of 100. These rates may be affected by the subtype and stage of Hodgkin lymphoma and the age and gender of the patient.
The 5-year survival rate for all people with Hodgkin lymphoma is 87%. If the cancer is found in its earliest stages, the 5-year survival rate is 91%. If cancer spreads regionally, the 5-year survival rate is 94%. If cancer has spread to different parts of the body, the 5-year survival rate is 81%.
It is important to remember that statistics on the survival rates for people with Hodgkin lymphoma are an estimate. The estimate comes from annual data based on the number of people with this cancer in the United States.
Also, experts measure the survival statistics every 5 years. So the estimate may not show the results of better diagnosis or treatment available for less than 5 years. Talk with your doctor if you have any questions about this information.