Prostate Cancer: Introduction, Risk Factors, Prevention, Screening, Symptoms and Signs
Prostate cancer is the most common cancer among men, except for skin cancer.
Prostate Gland
The prostate is a walnut-sized gland located behind the base of the penis, in front of the rectum, and below the bladder. It surrounds the urethra, the tube-like channel that carries urine and semen through the penis. The prostate’s main function is to make seminal fluid, the liquid in semen that protects, supports and helps transport sperm.
The prostate continues to enlarge as people age. This can lead to a condition called benign prostatic hypertrophy (BPH), which is when the urethra becomes blocked. BPH is a common condition associated with growing older, and it has not been associated with a greater risk of having prostate cancer.
Prostate Cancer
Cancer begins when healthy cells in the prostate change and grow out of control, forming a tumor. Prostate cancer is somewhat unusual when compared with other types of cancer.
This is because many prostate tumors do not spread quickly to other parts of the body. Some prostate cancers grow very slowly and may not cause symptoms or problems for years or ever.
Even when prostate cancer has spread to other parts of the body, it often can be managed for a long time. So people with prostate cancer, and even those with advanced prostate cancer, may live with good health and quality of life for many years.
However, if cancer cannot be well controlled with existing treatments, it can cause symptoms like pain and fatigue and can sometimes lead to death. An important part of managing prostate cancer is monitoring it for growth over time, to find out if it is growing slowly or quickly. Based on the pattern of growth, your doctor can decide the best available treatment options and when to give them.
Histology is how cancer cells look under a microscope. The most common histology found in prostate cancer is called adenocarcinoma. Other, less common histologic types include neuroendocrine prostate cancer and small cell prostate cancer. These rare variants tend to be more aggressive, produce much less PSA, and spread outside the prostate earlier.
Prostate Specific Antigen (PSA)
Prostate-specific antigen (PSA) is a protein produced by cells in the prostate gland and released into the bloodstream. PSA levels are measured using a blood test. Although there is no such thing as a “normal PSA” for anyone at any given age, a higher-than-normal level of Prostate-specific antigen (PSA) can be found in people with prostate cancer.
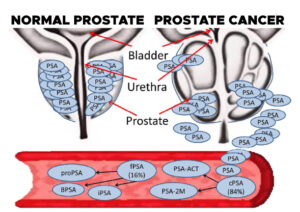
Other non-cancerous prostate conditions, such as BPH (see above) or prostatitis can also lead to an elevated PSA level. Prostatitis is the inflammation or infection of the prostate. In addition, some activities like ejaculation can temporarily increase prostate-specific antigen (PSA) levels.
Ejaculations should be avoided before a prostate-specific antigen (PSA) test to avoid falsely elevated tests. People should discuss with their primary care doctor the pros and cons of prostate-specific antigen (PSA) testing before using it to screen for prostate cancer.
Prostate Cancer Risk Factors
A risk factor is anything that increases a person’s chance of developing cancer. Although risk factors often influence the chance to develop cancer, most do not directly or by themselves cause cancer.
Some people with several known risk factors never develop cancer, while others with no known risk factors do. Knowing your risk factors and talking about them with your doctor may help you make more informed lifestyle and health care choices.
The following factors may raise a man’s risk of developing prostate cancer:
- The risk of prostate cancer increases with age, especially after age 50. Around 60% of prostate cancers are diagnosed in people who are 65 or older. Older adults who are diagnosed with prostate cancer can face unique challenges, specifically about cancer treatment.
- Black men in the United States, and other men of African ancestry, are diagnosed with prostate cancer more than men of other races. Black men are more likely to die from prostate cancer than white men.
- North American or northern European location. Prostate cancer occurs most often in North America and northern Europe. It also appears that prostate cancer is increasing among Asian people living in urbanized environments, such as Hong Kong, Singapore, and North American and European cities, particularly among those who have a lifestyle with less physical activity and a less healthy diet.
- Family history. Prostate cancer that runs in a family, called familial prostate cancer, makes up about 20% of all prostate cancers. This type of prostate cancer develops because of a combination of shared genes and shared environmental or lifestyle factors.
- Hereditary prostate cancer, which is inheriting the risk from a relative, is rare and accounts for about 5% of all cases. Hereditary prostate cancer occurs when changes in genes, or mutations, are passed down within a family from 1 generation to the next. Hereditary prostate cancer may be suspected if a family history includes any of the following characteristics:
- 3 or more first-degree relatives with prostate cancer
- Prostate cancer in 3 generations on the same side of the family
- 2 or more close relatives, such as a parent, sibling, child, grandparent, uncle, or nephew, on the same side of the family, diagnosed with prostate cancer before age 55
If someone has a first-degree relative – meaning a parent, sibling, or child – with prostate cancer, their risk of developing prostate cancer is 2 to 3 times higher than the average risk. This risk increases even further with the number of relatives diagnosed with prostate cancer.
- Hereditary breast and ovarian cancer (HBOC) syndrome. HBOC is associated with germline, or inherited, DNA-repair mutations to the BRCA1 and/or BRCA2 genes. BRCA stands for “BReast CAncer.” HBOC is most commonly associated with an increased risk of breast and ovarian cancers in women. However, people with HBOC also have an increased risk of developing breast cancer and a more aggressive form of prostate cancer. Mutations in the BRCA1 and BRCA2 genes are thought to cause only a small percentage of inherited prostate cancers. Those who have BRCA1 or BRCA2 mutations should consider screening for prostate cancer at an earlier age. Genetic testing may only be appropriate for families with prostate cancer that may also have HBOC.
- Other genetic changes. Other genes that may carry an increased risk of developing prostate cancer include HPC1, HPC2, HPCX, CAPB, ATM, FANCA, HOXB13, and mismatch repair genes. However, none of them has been directly shown to cause prostate cancer or be specific to this disease. Research to identify genes associated with an increased risk of prostate cancer is ongoing, and researchers are constantly learning more about how specific genetic changes can influence the development of prostate cancer. At present, there are no genetic tests available to determine someone’s chance of developing prostate cancer.
- Agent Orange exposure. The U.S. Department of Veterans Affairs (VA) lists prostate cancer as a disease associated with exposure to Agent Orange, a chemical used during the Vietnam War. If you are a veteran who may have been exposed to Agent Orange, please talk to your doctor in the VA system
- Eating habits. No study has proven that diet and nutrition can directly cause or prevent the development of prostate cancer. However, many studies that look at links between certain eating behaviors and cancer suggest there may be a connection. For example, obesity is associated with many cancers, including prostate cancer, and a healthy diet to avoid weight gain is recommended.
Prostate Cancer Prevention
Different factors cause different types of cancer. Researchers continue to look into what factors cause prostate cancer, including ways to prevent it. Although there is no proven way to completely prevent prostate cancer, you may be able to lower your risk.
1. Chemoprevention
A class of drugs called 5 alpha reductase inhibitors (5-ARIs), which include dutasteride (Avodart) and finasteride (Proscar), are often used to treat benign prostatic hypertrophy (BPH). They may also lower a man’s risk of developing prostate cancer. Some previous clinical trials suggested that 5-ARIs were linked to more aggressive prostate cancers, but newer studies have suggested that this is not true.
According to the results of a long-term follow-up study published in 2013, 78% of people either taking finasteride or placebo were still alive 15 years later. These results suggest that taking finasteride does not lower the risk of death for those with prostate cancer.
The U.S. Food and Drug Administration (FDA) has not approved these drugs for the prevention of prostate cancer. However, a 5-ARI is approved by the FDA for the treatment of lower urinary tract symptoms associated with benign prostatic hypertrophy (BPH).
The decision to take a 5-ARI is different for each person. Anyone considering taking this class of medication should discuss the possible benefits and side effects with their doctor.
2. Dietary Changes
There is not enough information right now to make clear recommendations about the exact role eating behaviors play in prostate cancer. Dietary changes may need to be made many years earlier in a person’s life to reduce the risk of developing prostate cancer later in life.
Here is a summary of the current research:
- In some studies, regularly eating foods high in fat, especially animal fat, has been associated with increased prostate cancer risk. However, no prospective studies have yet proven that diets high in animal fat raise the risk of prostate cancer. Prospective studies look at people who follow either high-fat or low-fat diets and then measure the total number of people in each group who are diagnosed with prostate cancer.
- A diet high in vegetables, fruits, and legumes, such as beans and peas, may lower the risk of prostate cancer. It is unclear which nutrients are directly responsible. Although lycopene, a nutrient found in tomatoes and other vegetables, is associated with a lower risk of prostate cancer, the data have not proven that there is a relationship between lycopene and preventing cancer.
- Currently, no specific vitamins, minerals, or other supplements have been shown in clinical trials to prevent prostate cancer. Talk with your doctor before taking any supplements to prevent prostate cancer.
- Specific changes to eating behaviors may not stop or slow the development of prostate cancer. It is possible such changes would need to be made early in life to affect.
Prostate Cancer Screening
Screening is used to look for cancer before you have any symptoms or signs. When cancer is found earlier in its development, it is often at an earlier stage.
This means that there is a better chance of successfully treating cancer. Scientists have developed, and continue to develop, tests that can be used to screen a person for specific types of cancer.The overall goals of cancer screening are to:
- Lower the number of people who die from the disease, or eliminate deaths from cancer altogether
- Lower the number of people who develop the disease
Screening for prostate cancer is done to find evidence of cancer in otherwise healthy adults. Two tests are commonly used to screen for prostate cancer:
- Digital rectal examination (DRE). A prostate exam is a test in which the doctor inserts a gloved, lubricated finger into the rectum and feels the surface of the prostate through the bowel wall for any irregularities.
- Prostate-specific antigen (PSA) blood test. There is controversy about using the prostate-specific antigen (PSA) test to look for prostate cancer in people with no symptoms of the disease. On the one hand, the PSA test is useful for detecting early-stage prostate cancer, especially in those with many risk factors, which helps some get the treatment they need before cancer grows and spreads. On the other hand, prostate-specific antigen (PSA) screening may find very slow-growing prostate cancers that would never threaten someone’s life. As a result, screening for prostate cancer using prostate-specific antigen (PSA) may lead to treatments that are not needed, which can cause side effects and seriously affect a person’s quality of life.
American Society of Clinical Oncology (ASCO) recommends that people with no symptoms of prostate cancer and who are expected to live less than 10 years do not receive PSA screening.
For those expected to live longer than 10 years, ASCO recommends that they talk with their doctor to find out if the test is appropriate for them.
Other organizations have different recommendations for screening:
- The U.S. Preventive Services Task Force (USPSTF) recommends that adults between 55 and 69 should discuss the pros and cons of PSA screening with their doctor before deciding about screening. People who are 70 and older should not have routine PSA screenings for prostate cancer.
- Both the American Urological Association and the American Cancer Society recommend that people be told the risks and benefits of testing before PSA screening occurs and then make an informed decision in consultation with their doctor.
- The National Comprehensive Cancer Network (NCCN) considers a patient’s age, PSA value, DRE results, and other factors in their recommendations.
It is not easy to predict which tumors will grow and spread quickly and which will grow slowly. Everyone should discuss with their doctor the pros and cons of prostate cancer screening based on their situation and personal risk of prostate cancer, so they can work together to make an informed decision.
Prostate Cancer Symptoms and Signs
The symptoms and signs of prostate cancer may include:
- Frequent urination
- Weak or interrupted urine flow or the need to strain to empty the bladder
- The urge to urinate frequently at night
- Blood in the urine
- New onset of erectile dysfunction
- Pain or burning during urination, which is much less common
- Discomfort or pain when sitting, caused by an enlarged prostate
Other noncancerous conditions of the prostate, such as benign prostatic hypertrophy (BPH) or an enlarged prostate, can cause similar symptoms.
Or, the cause of a symptom may be a different medical condition that is also not related to cancer. Urinary symptoms also can be caused by an infection of the bladder or other conditions.
If cancer has spread outside of the prostate gland, symptoms may include:
- Pain in the back, hips, thighs, shoulders, or other bones
- Swelling or fluid buildup in the legs or feet
- Unexplained weight loss
- Fatigue
- Change in bowel habits
If you are concerned about any changes you experience, please talk with your doctor.
Your doctor will ask how long and how often you have been experiencing the symptom(s), in addition to other questions. This is to help figure out the cause of the problem, called a diagnosis.
If prostate cancer is diagnosed, relieving symptoms remains an important part of cancer care and treatment. This may be called palliative care or supportive care.
It is often started soon after diagnosis and continued throughout treatment. Be sure to talk with your health care team about the symptoms you experience, including any new symptoms or a change in symptoms.